Hypoxic-Ischemic Encephalopathy Lawyer
Compassionate Support for Families Facing HIE Birth Injuries
Bringing a new life into the world is a moment of joy and hope. However, when complications arise, such as hypoxic-ischemic encephalopathy (HIE), the experience can turn into a distressing ordeal. HIE, often referred to as birth asphyxia or neonatal encephalopathy, is a serious condition caused by inadequate oxygen and blood flow to a baby’s brain around the time of birth.
While HIE can occur without negligence, medical errors and oversight can play a significant role in many cases. If a healthcare provider fails to adhere to the standard of care, and this failure results in HIE, it may be considered medical malpractice. As devastating as a neonatal hypoxic-ischemic encephalopathy diagnosis can be, it’s crucial to understand that you are not alone.
At American Baby and Child (ABC) Law Centers, Reiter & Walsh, we focus on supporting families affected by HIE resulting from medical negligence. Our dedicated HIE lawyers are deeply knowledgeable about the complexities of birth injury cases and are committed to advocating for the rights of your HIE baby. We understand the emotional and financial burdens that come with an HIE diagnosis, and we are here to help you navigate this challenging journey.
Why Choose an HIE Lawyer from ABC Law Centers?
Our birth injury attorneys at ABC Law Centers are committed to holding medical professionals accountable and securing the resources your family needs for your HIE baby’s future. We will stand by your side, offering compassionate guidance and relentless advocacy every step of the way.
Our experienced birth trauma litigation group can provide invaluable assistance by:
- Investigating the circumstances surrounding the birth to identify potential medical negligence or malpractice.
- Securing expert medical testimony to establish the link between negligence and the HIE diagnosis.
- Pursuing compensation to cover medical expenses, ongoing care, and other related costs to ensure your child receives the best possible support and treatment.
This isn’t a path you have to walk alone. A birth injury lawsuit can help secure financial compensation to ensure your child’s medical needs are met. Contact us today for a free case review.
What is Hypoxic-Ischemic Encephalopathy?
Hypoxic-ischemic encephalopathy (HIE) is a type of brain dysfunction or brain damage caused by insufficient oxygenated blood flow during or near the time of birth. Terms that are sometimes used as synonyms for HIE include birth asphyxia and neonatal encephalopathy, although technically these have distinct meanings.
If a baby is diagnosed with HIE, it is critical that doctors administer therapeutic hypothermia very shortly after birth/the oxygen-depriving incident. This treatment can minimize the extent of permanent brain damage, and reduces the risk of resultant disabilities such as cerebral palsy.

Causes of Birth Asphyxia and HIE
There are many potential causes of HIE, including high-risk pregnancy conditions, labor and delivery issues, and medical mistakes. Usually, HIE can be prevented through careful fetal monitoring and timely intervention in response to complications. However, medical professionals may miss opportunities to prevent HIE or perform negligent actions that cause HIE.
Role of Medical Negligence in HIE
While HIE can occur without negligence, medical errors and oversight can play a significant role in many cases. If a healthcare provider fails to adhere to the standard of care, and this failure results in HIE, it may be considered medical malpractice.
Potential negligent causes of hypoxic-ischemic encephalopathy (HIE) may include:
- Failure to Monitor: Inadequate fetal monitoring during labor and delivery can result in missed signs of distress.
- Delayed Response: Delays in performing necessary interventions, such as an emergency C-section, can lead to HIE.
- Medical Errors: Misuse of delivery tools, improper administration of anesthesia, or failure to address high-risk conditions promptly can contribute to HIE.
Specific complications and medical mistakes that can lead to perinatal asphyxia or hypoxic-ischemic encephalopathy include, among others:
- Abnormal fetal position/presentation
- Anesthesia errors
- Birth trauma
- C-section errors and delays
- Cephalopelvic disproportion (CPD)
- Fetal monitoring errors and failure to recognize signs of fetal distress (oxygen deprivation)
- Fetal stroke
- Forceps and vacuum extractor injuries
- A high-risk pregnancy (e.g. one involving gestational diabetes, preeclampsia, or obesity), especially if mismanaged
- Infections in newborns
- Intracranial hemorrhages (brain bleeds)
- Kernicterus
- Low birth weight (LBW)
- Macrosomia
- Maternal infections
- Meconium aspiration syndrome (MAS)
- Neonatal breathing mismanagement
- Oligohydramnios
- Placental complications:
- Polyhydramnios
- Postterm pregnancy
- Premature rupture of membranes (PROM)
- Preterm birth
- Prolonged and arrested labor
- Umbilical cord issues:
- Vasa previa
- Uterine tachysystole/hyperstimulation (this often results from the misuse of contraction-enhancing drugs called Pitocin and )
- Twins/multiples
- Vaginal birth after cesarean (VBAC)
For more detailed information on the causes and risk factors for hypoxic-ischemic encephalopathy.
Signs and Symptoms of HIE
Understanding the signs and symptoms of hypoxic-ischemic encephalopathy is crucial for early diagnosis and intervention. Recognizing these indicators promptly can significantly impact the outcomes for newborns affected by this condition. HIE manifests through a range of neurological signs, from subtle to severe.
Signs of hypoxic-ischemic encephalopathy at birth may include the following:
- Breathing problems/need for resuscitation of the newborn
- Low APGAR Scores. An APGAR score assesses the overall health of a newborn over the first few minutes of life. It assigns scores to conditions such as the baby’s skin color and complexion, pulse rate, reflexes, muscle tone, and breathing.
- Seizures shortly after birth
- Difficulty feeding, including the inability to latch, suck, or swallow
- Abnormal neonatal reflexes (e.g. the baby fails to respond to loud sounds or movement, does not grasp onto objects such as a finger, etc.)
- Profound metabolic or mixed acidemia in an umbilical artery blood sample (the baby’s blood is acidic/has a low ph)
- Hypotonia (low muscle tone/limpness)
- Multiple organ problems (e.g., the involvement of the lungs, liver, heart, intestines)
- Coma/altered consciousness
Important note: HIE can sometimes be recognized while the baby is still in utero by looking for signs of fetal distress.
Diagnosing Hypoxic-Ischemic Encephalopathy
Diagnosis of perinatal asphyxia involves clinical evaluation, Apgar scoring, blood tests and blood gas analysis to assess oxygen levels, and neuroimaging studies to evaluate brain injury. Immediate management focuses on providing adequate oxygenation, respiratory support, and therapeutic hypothermia (cooling therapy) to reduce brain damage.
Tests may include the following:
- CT scans
- PET scans
- MRIs
- Blood glucose tests
- Umbilical cord and arterial blood gas tests
- EEGs
- Ultrasounds
If delivery was traumatic, oxygen-depriving complications occurred, or the baby showed signs of HIE, medical professionals should begin the diagnostic process.
It is important to note that a newborn may have sustained a hypoxic-ischemic injury, but not show signs of it until later in childhood when they exhibit delayed developmental milestones (including problems with motor skills, growth, cognitive function, etc.).
HIE can cause numerous health conditions, including:
- Seizure disorders
- Cerebral palsy (CP)
- Learning disabilities
- Motor disorders
- Microcephaly
- Speech and language problems
- Vision and hearing impairments
- Sensory processing disorders
Treatments for Hypoxic-Ischemic Encephalopathy
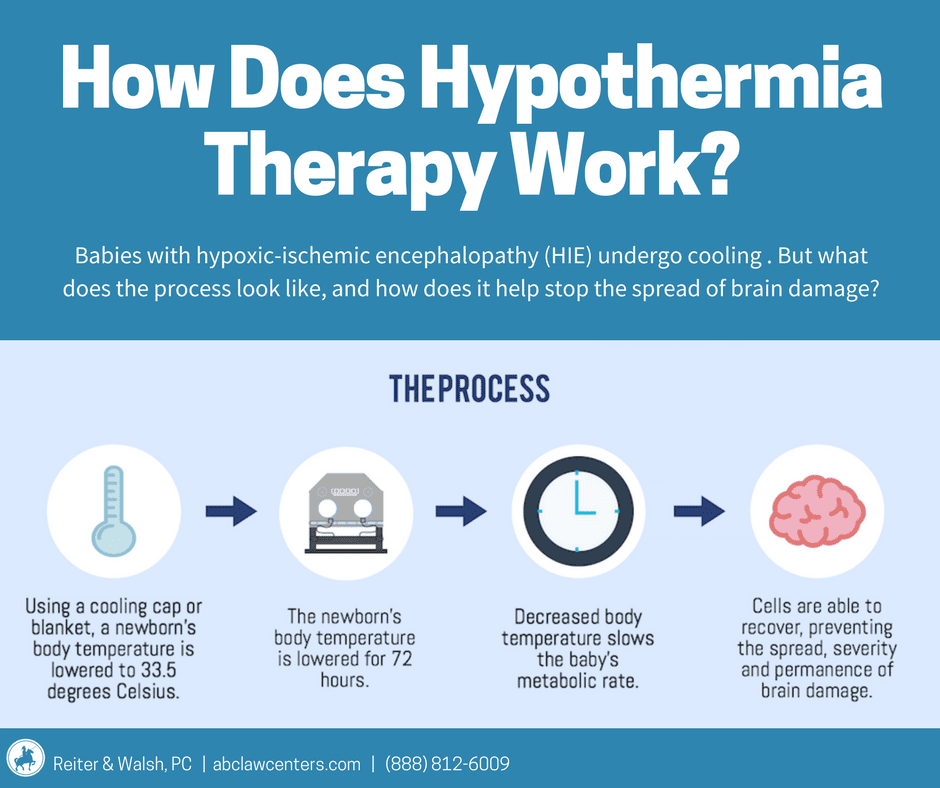
Babies with HIE may require a variety of different treatments. One of the most important is therapeutic hypothermia (brain/body cooling), which has been shown to improve survival rates and minimize the extent of permanent brain damage in babies with HIE. It also reduces the risk of the child developing disabilities such as cerebral palsy.
Therapeutic hypothermia consists of lowering a newborn’s temperature to around 92-94 degrees Fahrenheit for a period of about 72 hours. This slows the baby’s metabolic rate, which allows cells time to recover and reduces the spread of damage.
Therapeutic hypothermia must begin as soon as possible (it is most effective if begun within the first six hours after injury), as long as the baby meets eligibility criteria. Failure to perform therapeutic hypothermia on a newborn baby who is eligible and in need of the treatment is an instance of medical malpractice.
Preventing Hypoxic-Ischemic Encephalopathy
Prevention of birth asphyxia and HIE boils down to two major components:
- Closely monitoring the mother and baby so that fetal distress or impending distress is recognized.
- Quickly delivering the baby when fetal distress or impending distress are present.
During pregnancy, the mother and baby should have regular prenatal tests to help ensure fetal health. If the pregnancy is high-risk, more frequent prenatal testing is required and the mother should be referred to a maternal-fetal specialist. As soon as the mother is admitted to the labor and delivery unit, a fetal heart monitor should be attached to her body and the baby’s heart rate should be continuously monitored.
The point of a fetal heart monitor is to alert the medical team of fetal distress. If a baby is experiencing a lack of oxygen to the brain, this will result in “nonreassuring heart tracings” on the fetal monitor. When nonreassuring tracings occur, the medical team may try resuscitative maneuvers, which are aimed at increasing blood flow and oxygen to the baby. These maneuvers may include giving the mother IV fluids or oxygen, or changing her position. However, there is no guarantee that resuscitative maneuvers will relieve fetal distress. In fact, distress caused by certain obstetrical conditions, such as complete umbilical cord compression or complete placental abruption may not be affected by in-utero resuscitation; babies experiencing these conditions must be delivered within a matter of minutes.
When fetal distress occurs or is impending (i.e. a pregnancy/delivery complication has been identified), the medical team should make preparations for a possible emergency C-section while doing in-utero resuscitation maneuvers. It is very important to have highly experienced members of the healthcare team involved in labor and delivery. It takes skill to interpret fetal heart tracings, and these tracings are often the only indication that a baby is experiencing birth asphyxia and HIE. The team also must be well-coordinated so that preparations and execution of a C-section delivery are fast. A delay in performing a necessary C-section can cause HIE and permanent brain damage in the baby.
What is the Incidence of HIE?
Hypoxic-ischemic encephalopathy (HIE) is estimated to occur in about 1.5 per 1,000 live births, although this estimate may be imprecise. It accounts for 23% of neonatal deaths worldwide, and babies that survive may develop cerebral palsy (CP), intellectual and developmental disabilities (I/DDs), epilepsy, and many other associated conditions.
How Serious is HIE?
Hypoxic-ischemic encephalopathy (HIE) can be categorized into different levels based on its severity – mild HIE, moderate HIE, and severe HIE. The severity of HIE is typically assessed based on clinical criteria, such as the extent of neurological symptoms and the results of diagnostic tests like MRI or EEG. The classification into different levels helps healthcare providers determine the appropriate treatment and predict long-term outcomes for the affected newborn.
For babies with HIE, the seriousness of the brain damage (and the likelihood of subsequent disabilities) depends on the following conditions:
- The severity of the oxygen deprivation
- The length of time that the baby was deprived of oxygen
- The condition of the baby prior to the oxygen deprivation
- The management of the baby by the medical team after the oxygen-depriving event occurred
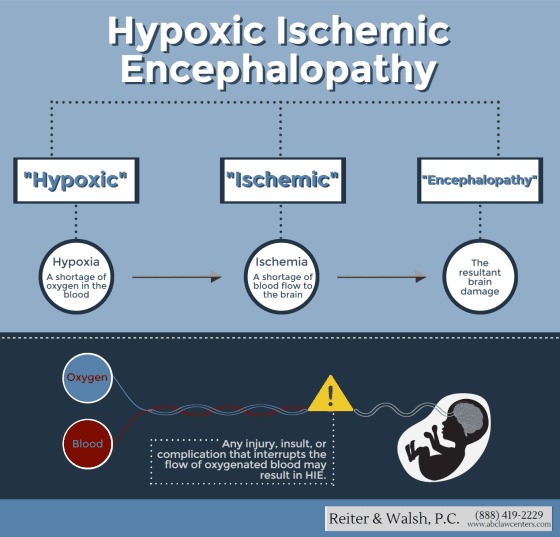
Breaking Down ‘Hypoxic-Ischemic Encephalopathy’: What Is a Hypoxic-Ischemic Brain Injury?
Hypoxic-ischemic injury occurs when the baby’s brain is deprived of oxygenated blood. “Hypoxic/hypoxia” refers to a lack of oxygen, and “ischemic/ischemia” refers to a lack of blood flow. In older children and adults, HIE may result from anything that causes a lack of oxygen to the brain including a heart attack, stroke, trauma to the head, carbon monoxide poisoning, drug overdose, or near drowning. In babies, HIE can be due to problems during pregnancy, labor and delivery, or shortly after birth.
Frequently asked question: how long can a baby survive without oxygen?
The question of how long an unborn baby can survive without oxygen is a complex one. First, there is a distinction between survival with adverse health effects (such as brain damage) versus survival without adverse health effects. Second, it depends on the severity of the oxygen deprivation. If the baby is receiving no or very little oxygen, they could die or become seriously brain injured in a matter of minutes. Often, the safest and quickest way to save a baby that is being deprived of oxygen is via emergency C-section.
Guidelines from the American College of Obstetricians and Gynecologists (ACOG) state that an emergency C-section must be performed within 30 minutes from the time it is determined to be necessary. However, there are many situations in which this is not fast enough, and it is against standard of care to delay an emergency C-section more than is absolutely necessary. In many cases, the decision-to-delivery interval should only be a few minutes (5).
Frequently asked question: can hypoxia cause seizures?
Yes, HIE can cause neonatal seizures as well as long-term seizure disorders such as epilepsy. When oxygen deprivation occurs, brain cells begin to die, and the complex connections between different parts of the brain are disrupted. This can result in seizures, which are abnormal electrical discharges in the brain.
Visualizing HIE and Neonatal Brain Injury
HIE and diminished blood flow
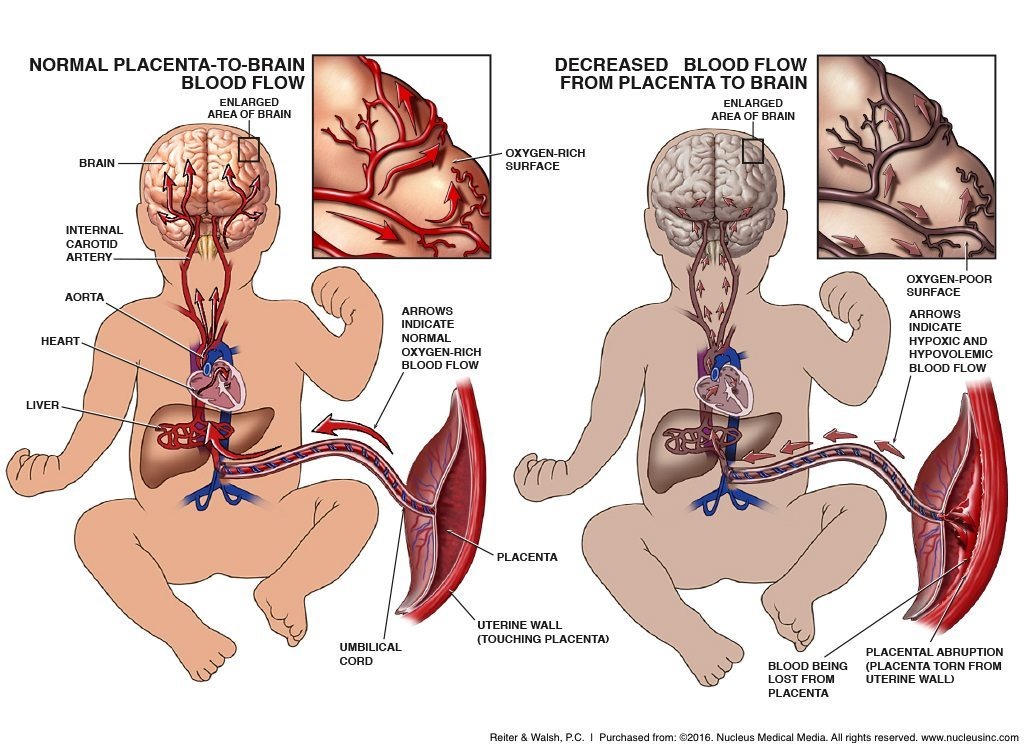
Relevant terms and definitions
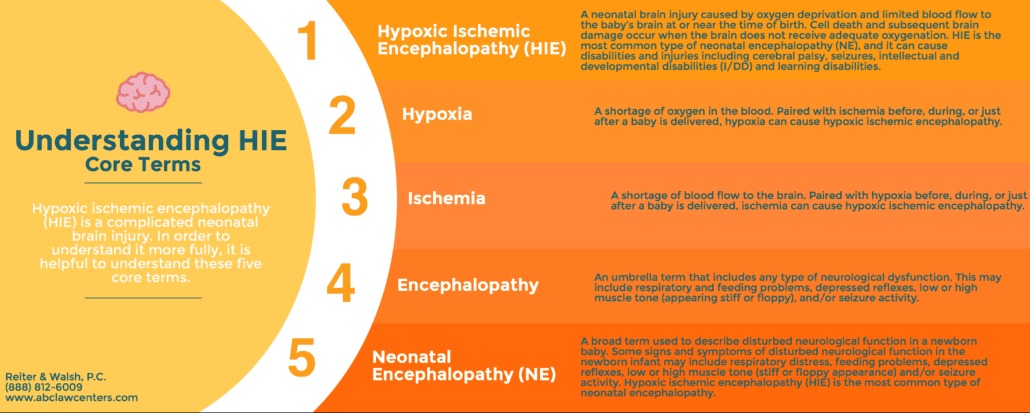



Contact a Hypoxic Ischemic Encephalopathy Lawyer from ABC Law Centers Today
Hypoxic-ischemic encephalopathy cases require specific, extensive knowledge of both law and medicine. For the best case outcomes, it’s critical to find an attorney and a birth injury litigation law firm that focuses specifically on birth injury and HIE cases. At ABC Law Centers: Birth Injury Lawyers, our attorneys have been focusing their careers on this area of law, and they consistently secure multi-million dollar settlements for their clients.
Our office is located near Detroit, Michigan, but we handle cases throughout the United States. Our birth injury team is also equipped to handle cases involving military medical malpractice and federally funded clinics.
Contact us today to begin your free case review. We will answer your legal questions, determine the negligent party, and inform you of your legal options. Moreover, you pay nothing throughout the entire legal process unless we win or favorably settle your case.
Featured Videos
Posterior Position
Hypoxic-Ischemic Encephalopathy (HIE)

Featured Testimonial
What Our
Clients Say…
After the traumatic birth of my son, I was left confused, afraid, and seeking answers. We needed someone we could trust and depend on. ABC Law Centers: Birth Injury Lawyers was just that.
- Michael
Helpful resources
Legal help: our HIE lawyers and firm
- Kurinczuk, J. J., White-Koning, M., & Badawi, N. (2010). Epidemiology of neonatal encephalopathy and hypoxic–ischaemic encephalopathy. Early human development, 86(6), 329-338.
- What is the global prevalence of hypoxic-ischemic encephalopathy (HIE)? (2018, July 26). Retrieved November 15, 2018, from https://www.medscape.com/answers/973501-106461/what-is-the-global-prevalence-of-hypoxic-ischemic-encephalopathy-hie
- Heinz, U. E., & Rollnik, J. D. (2015). Outcome and prognosis of hypoxic brain damage patients undergoing neurological early rehabilitation. BMC research notes, 8(1), 243.
- (n.d.). Retrieved November 15, 2018, from https://www.uptodate.com/contents/hypoxic-ischemic-brain-injury-in-adults-evaluation-and-prognosis
- Reiter, J., P.C. (2008, July). Emergency Cesarean Sections: When 30 Minutes Is Not Fast Enough. BTLG Newsletter.
- (n.d.). Retrieved November 15, 2018, from https://www.uptodate.com/contents/clinical-features-diagnosis-and-treatment-of-neonatal-encephalopathy#H16


