Placental Abruption During Labor & Delivery
Disclaimer: Please know that our website is owned by a medical malpractice law firm that focuses exclusively on birth injury cases. We try to provide useful medical information to our readers, but we cannot provide treatments or medical advice. If you need medical help or advice, please contact your doctor or call 911/your country’s emergency number.
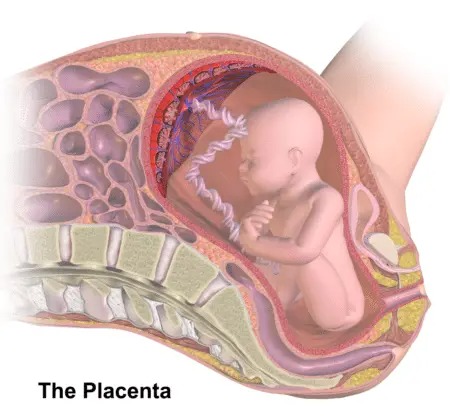
Under normal circumstances, the placenta is attached to the uterine wall, providing the baby with nutrients and oxygen as well as removing fetal waste products. It is usually expelled naturally after the baby is delivered as part of the “afterbirth.”
What is placental abruption?
Placental abruption happens when the placenta separates prematurely from the uterine wall. It usually occurs in the third trimester, but can occur as early as 20 weeks gestation. Placental abruption occurs in about one percent of pregnancies (1).
When this happens, the baby can stop receiving adequate oxygen. Even cases of partial placental abruption (when the placenta is not completely detached) can progress and become severe very quickly, so physicians should carefully monitor the situation and be prepared for an emergency C-section. If a necessary C-section is delayed, the baby may experience birth asphyxia and sustain forms of brain damage such as hypoxic-ischemic encephalopathy (HIE) and cerebral palsy (CP).
Risk factors & causes of placental abruption
There are a number of conditions and risk factors associated with placental abruption. These can include (1, 2):
- Maternal hypertension (preeclampsia or high blood pressure)
- Trauma to the abdomen
- Rupture of membranes (mother’s water breaks)
- Chorioamnionitis
- Pregnancy with multiples
- Previous placental abruption
- Advanced maternal age (over 35)
- Abnormalities in the uterus
- Smoking
- Induction of labor
- Intrauterine growth restriction (IUGR)
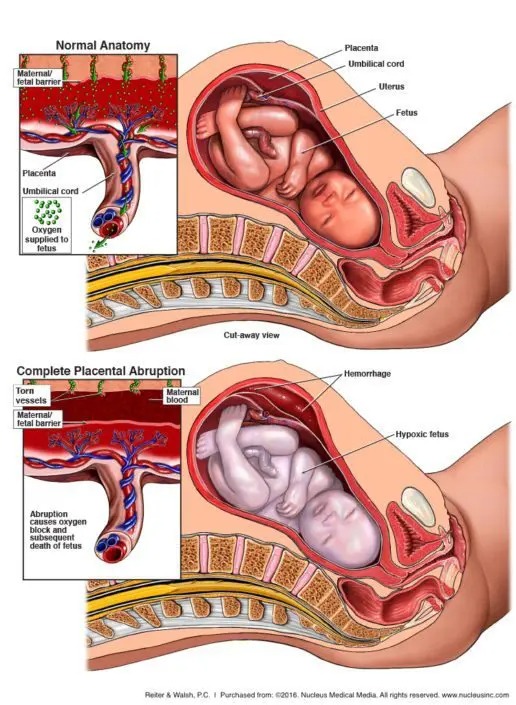
Placental abruption with fetal hypoxia
Signs & Symptoms of Placental Abruption
Signs and symptoms of placental abruption can include (1, 2):
- Vaginal bleeding (however, 20 percent of women will not experience bleeding)
- Rapid contractions or uterine irritability
- Uterine pain or tenderness
- Abdominal pain
- Fetal heart rate abnormalities
- Back pain
Any amount of vaginal bleeding during pregnancy should be documented and assessed by your medical caregiver as soon as possible. Excessive bleeding requires immediate emergency medical attention.
Any trauma to the abdomen during pregnancy should be assessed immediately!

Diagnosis of placental abruption
Caregivers should suspect and act on placental abruption based on the risk factors and symptoms described above.
Treatment for partial placental abruption
A patient with a partial placental separation must be closely monitored and the baby should be delivered emergently if the condition becomes non-reassuring.
Complications of placental abruption
Placental abruption can lead to the following (1, 2):
- Premature birth
- Low birth weight
- Fetal growth restriction
- Maternal blood loss
- Need for blood transfusion
- Blood clotting issues
- Maternal hemorrhage
- Fetus not getting enough oxygen*
- Fetal death
Birth injury law is all we do.
Secure your child’s future. Call the trusted birth injury attorneys at ABC Law Centers: Birth Injury Lawyers now.
What happens when a fetus doesn't get enough oxygen?*
Failure to quickly deliver a baby when a placental abruption occurs can cause the baby to experience severe oxygen deprivation (birth asphyxia), which can cause birth injuries such as:
- Hypoxic-ischemic encephalopathy (HIE): HIE usually involves damage to the basal ganglia, cerebral cortex, or watershed regions of the brain, but it sometimes includes periventricular leukomalacia (PVL)
- Neonatal encephalopathy
- Permanent brain injury
- Seizure disorders
- Cerebral palsy (CP)
- Developmental delays
- Learning disabilities
- Motor disorders
- Microcephaly
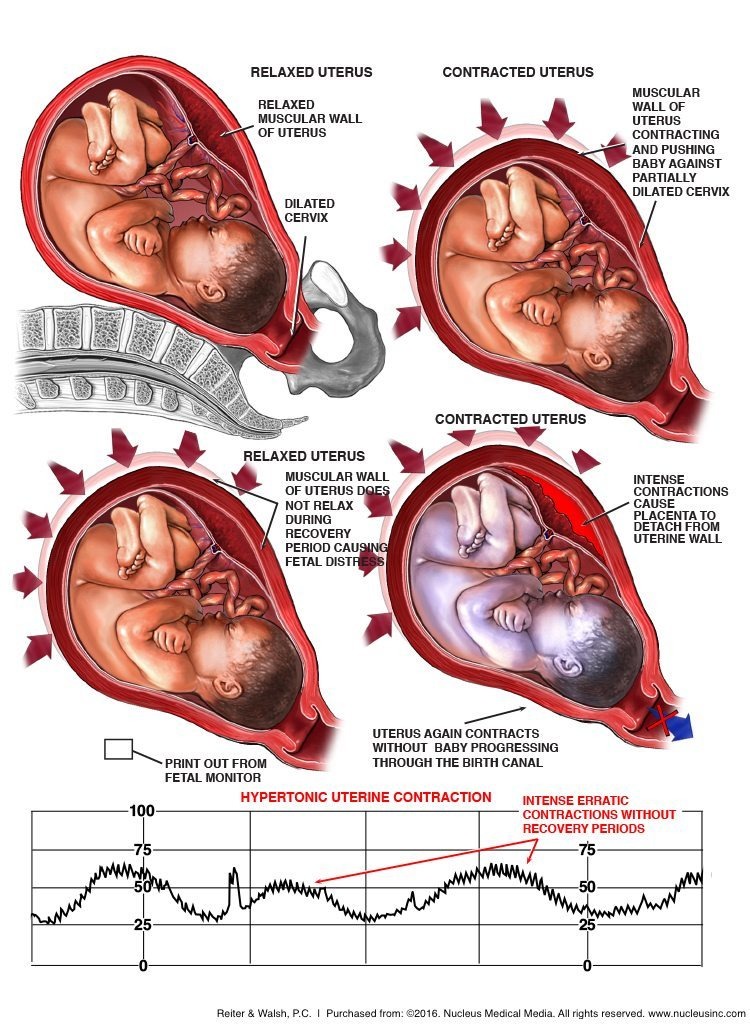
Excessive uterine contractions (hyperstimulation) with resultant placental abruption
Placental abruption, birth injury, and medical malpractice
Medical professionals should follow standard of care to minimize the chance of placental abruption (especially in women with risk factors), monitor the health of both mothers and babies, and promptly intervene if a placental abruption occurs. Failure to do these things is negligence, and if negligence causes harm, it constitutes medical malpractice.
A birth injury can be defined as any type of harm to a baby that occurs shortly before, during, or after delivery. In cases of placental abruption, babies may sustain birth injuries such as hypoxic-ischemic encephalopathy, cerebral palsy, and other forms of brain damage.
If your child has a birth injury caused by mismanaged placental abruption, they may be eligible for compensation through a birth injury lawsuit. This compensation can cover medical treatments, caretaking expenses, assistive technology (e.g. mobility equipment), and other forms of support they may require throughout their life.


Birth injury attorneys serving clients nationwide
ABC Law Centers: Birth Injury Lawyers was established in 1997, and specifically handles birth injury cases. Beyond our focus on delivering unparalleled legal services, our attorneys and staff work to build close, comforting, and openly communicative relationships with clients. At every step of the litigation process, our small, family-oriented team is there to support you and keep you informed. Although we’re based near Detroit, Michigan (in Bloomfield Hills), we’re equipped to handle these cases throughout the state of Michigan and around the country. The ABC Law Centers: Birth Injury Lawyers birth injury team has also handled FTCA cases involving military medical malpractice and federally-funded clinics.
Please reach out today to learn more. Clients pay nothing throughout the legal process unless we obtain financial recovery for them!
“When you see your child suffer because of someone’s mistake you want justice. As a mother you want someone in your corner to fight as hard as you would and I luckily found that in Jesse Reiter and his staff!” – Wendy, former client
Featured Videos
Posterior Position
Hypoxic-Ischemic Encephalopathy (HIE)

Featured Testimonial
What Our
Clients Say…
After the traumatic birth of my son, I was left confused, afraid, and seeking answers. We needed someone we could trust and depend on. ABC Law Centers: Birth Injury Lawyers was just that.
- Michael
Helpful resources
- Placental Abruption: Risks, Causes, Symptoms and Treatment. (2017, May 02). Retrieved February 18, 2019, from http://americanpregnancy.org/pregnancy-complications/placental-abruption/
- Placental abruption. (2018, January 12). Retrieved February 18, 2019, from https://www.mayoclinic.org/diseases-conditions/placental-abruption/symptoms-causes/syc-20376458


