Placenta Previa and Birth Injury
The placenta is an organ that supplies a baby with nutrients and oxygen and removes waste from the baby in the womb. Normally, the placenta is near the top or on the side of the uterus and makes its way through the birth canal after the baby has been delivered as part of the “afterbirth.”
Placenta previa is a condition in which the placenta lies unusually low in the uterus, where it partially or completely covers the mother’s cervix and may block the baby’s passage out of the womb. When diagnosed early in pregnancy, placenta previa is usually not a serious problem; as the baby grows, the placenta expands and lifts up and away from the cervix on its own. This is known as “placental migration.” Due to this, most cases of placenta previa resolve on their own before the third trimester.
However, in the third trimester, placenta previa can lead to life-threatening hemorrhagic bleeding in the mother and birth injuries to the baby. In many cases, placenta previa does not resolve and requires delivery by C-section. Placenta previa is estimated to occur in approximately one in every 200 pregnancies in the third trimester of pregnancy.
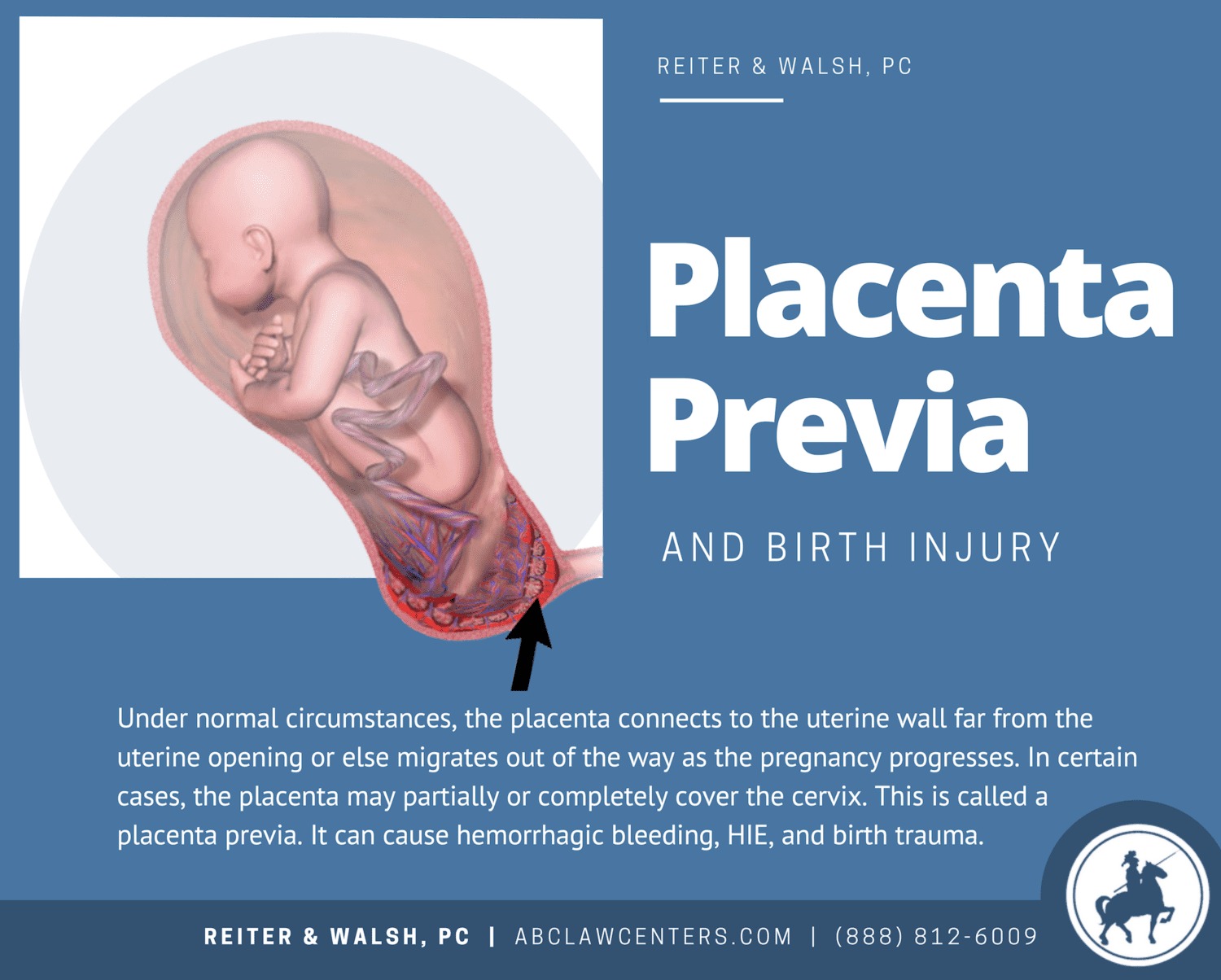
Types of Placenta Previa
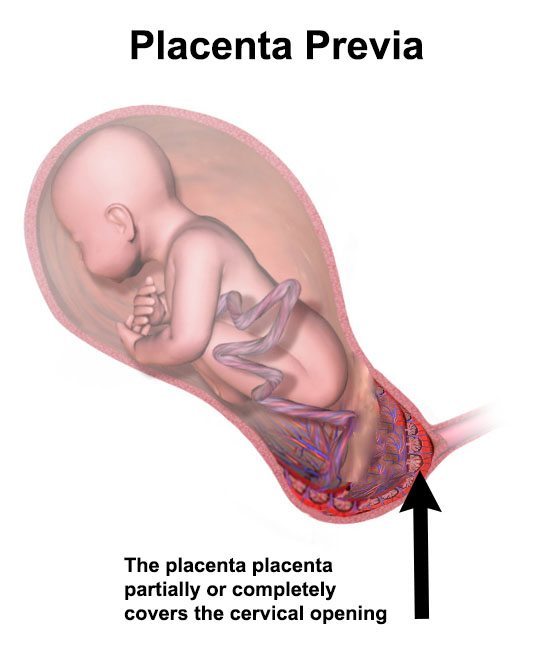
There are two types of placenta previa (1):
- Complete or total previa, in which the placenta covers the cervix entirely
- Marginal or partial previa, in which the placenta is on the border of the cervix
Signs and Symptoms of Placenta Previa
Typically, the first sign of placenta previa is painless bleeding during the second half of pregnancy. The bleeding can vary from minimal to profuse. Many women with placenta previa will stop bleeding and then begin again. Contractions may or may not be present. Placenta previa may also be suspected if the baby is in an abnormal position, the mother is experiencing premature contractions, or the uterus measures larger than it should be for gestational age.
If you experience any amount of bleeding during your pregnancy, call your doctor right away. If bleeding is severe, seek emergency care.
Risk Factors For Placenta Previa
The exact cause of placenta previa is unknown, although risk factors have been identified. They include:
- Having previously given birth
- Multiples pregnancy (twins, triplets, etc.): he risk of placenta previa was found to be 40% higher in twin births than in singleton births
- Previous surgeries involving the uterus, such as a C-section, surgery to remove uterine fibroids, or dilation and curettage (D&C): The risk increases with the number of surgeries involving the uterus
- Prior placenta previa: It can reoccur in 4-8% of subsequent pregnancies
- Being age 35 or older (“advanced maternal age”)
- Smoking or using cocaine
Our team is here to help.
Dealing with a birth injury diagnosis can be difficult, but our attorneys can help. Call us when you’re ready.
Diagnosing Placenta Previa
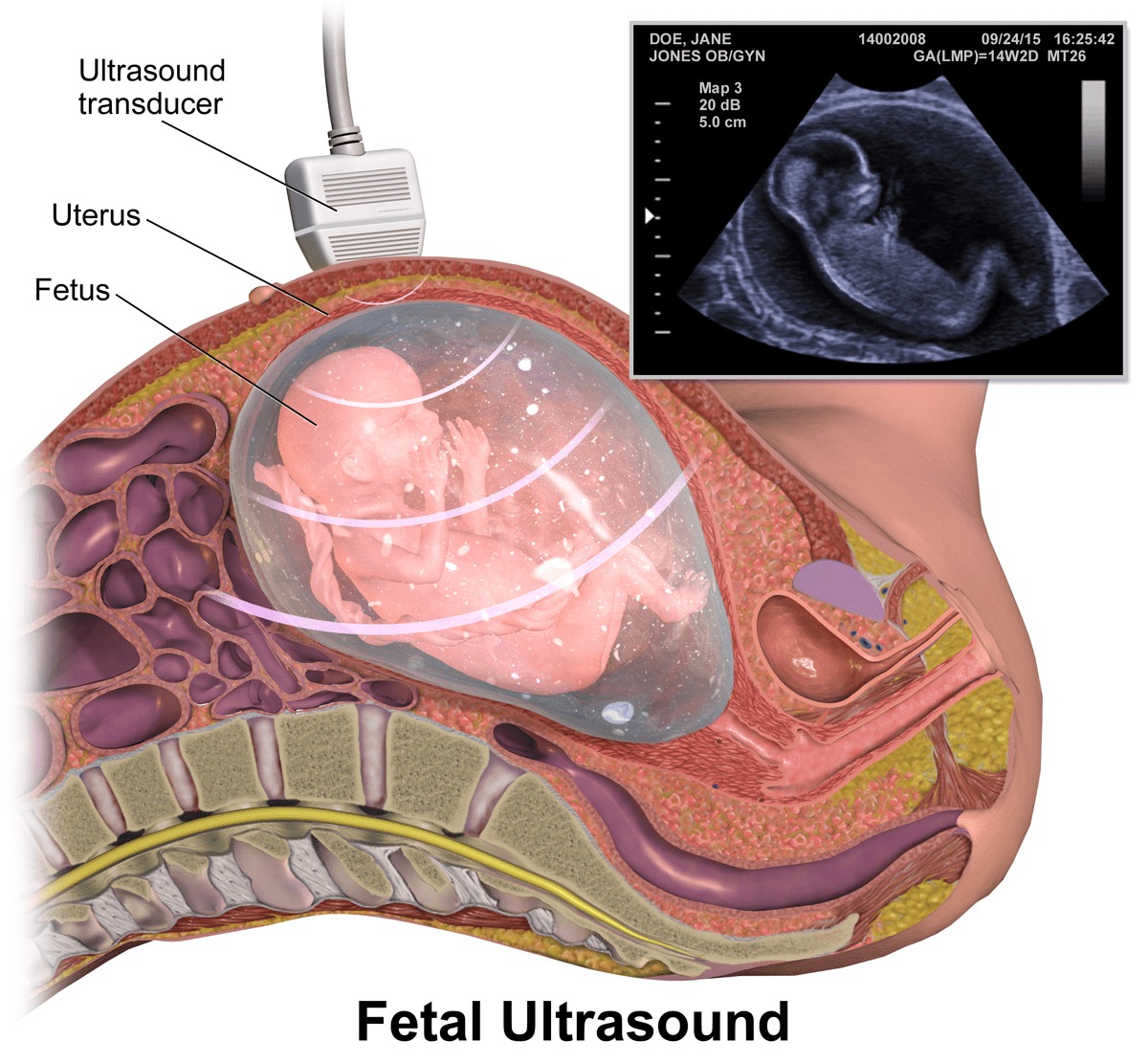
Placenta previa is diagnosed via ultrasound. It can be found during a routine prenatal ultrasound or during an ultrasound administered after vaginal bleeding occurs. Most cases of placenta previa are diagnosed during routine ultrasounds at 16-20 weeks.
Diagnosis may require a combination of abdominal ultrasound and transvaginal ultrasound. It is important that the doctor administers a transvaginal ultrasound with great care in cases of placenta previa because the ultrasound may cause more bleeding.
Placenta previa may also require additional ultrasounds during pregnancy to monitor the movement of the placenta.
Complications of Placenta Previa
During labor, the baby moves through the cervix into the birth canal. If the mother has placenta previa, the placenta is more likely to endure tearing as a result of contractions and the movement through the cervix. Therefore, placenta previa can lead to several complications that threaten the health of the mother and baby, such as:
- Preterm birth: Severe bleeding may prompt an emergency C-section before the baby reaches full-term. Roughly 15% of women with placenta previa deliver before 34 weeks gestation. This puts the baby at risk for complications related to premature birth.
- Bleeding during pregnancy: Severe, life-threatening vaginal bleeding can occur during labor, delivery, or after delivery in cases of placenta previa. In studies of women with placenta previa, 52% of them experienced antepartum bleeding, and 22% had postpartum hemorrhage.
- Placenta accreta: In cases of placenta previa, placenta accreta is more likely to occur. Placenta accreta is when the placenta is attached to the uterine wall and has trouble detaching during the afterbirth. Removing the placenta can cause hemorrhage. To control this bleeding, the patient may need multiple transfusions and a hysterectomy (full removal of the uterus). Placenta accreta can also lead to fetal hypoxia (birth asphyxia) resulting in hypoxic-ischemic encephalopathy (HIE).
- Placental abruption: This occurs when the placental lining has separated from the uterus before the baby is born. Because of the potential for tearing in placenta previa, placental abruption is more likely. Placental abruption can deprive the baby of oxygen and critical nutrients (possibly leading to HIE and other injuries), as well as cause heavy bleeding in the mother.
Treatment for Placenta Previa
The goal of treating placenta previa is to get the mother as close to the due date as possible and monitor her bleeding during that time. Possible treatment options for placenta previa include:
- More frequent monitoring
- Frequent hospital visits
- Bed rest
- Steroid shots to help mature the baby’s lungs (i.e. progesterone therapy)
- C-section (emergency C-section delivery if the mother’s bleeding cannot be controlled, or a scheduled C-section delivery)*
*Roughly 75% of women with placenta previa in their third trimester have planned C-section deliveries. Women with marginal placenta previa can deliver vaginally with close monitoring, but almost all women with complete placenta previas require a cesarean delivery.
Your physician may recommend you avoid the following things that could cause contractions or increase bleeding if you have placenta previa:
- Pelvic exams
- Travel
- Sexual intercourse
- Using tampons
- Douching
- Running
- Jumping
- Squatting
Tell us your story.
Call us today. There is never any fee unless we win or favorably settle your case.
Placenta Previa and Medical Malpractice
The serious nature of placenta previa requires careful evaluation, monitoring, and preparedness by an obstetrician. Failure to properly diagnose or treat placenta previa can be very dangerous for both mother and baby.
Some examples of situations that constitute medical malpractice in cases of placenta previa:
- Failure to perform an ultrasound to diagnose placenta previa
- Failure to continuously monitor the baby during an emergent placenta previa situation, resulting in fetal hypoxia to the baby
- Vaginal delivery attempted when complete previa exists
- Digital pelvic exam performed when complete previa is present, causing hemorrhaging
- Delayed emergency C-section


Get Legal Help
The award-winning attorneys at ABC Law Centers: Birth Injury Lawyers have over 100 years of combined experience in birth injury cases and focus exclusively on birth injury, including placenta previa cases. If you experienced placenta previa during your pregnancy and your child was physically or mentally injured as a result, we can help you. Our skilled attorneys and exceptional medical experts will work tirelessly to get you the compensation you and your family are entitled to for health care, medical expenses, special education, assistive devices, loss of income, and pain and suffering. We’ve helped clients across the United States receive compensation for lifelong care. We are located in Michigan, but serve clients in many parts of the U.S., and will travel to your hometown as necessary. We are devoted to the needs of our clients and do not charge for our legal processes unless we win your case.
Featured Videos
Posterior Position
Hypoxic-Ischemic Encephalopathy (HIE)

Featured Testimonial
What Our
Clients Say…
After the traumatic birth of my son, I was left confused, afraid, and seeking answers. We needed someone we could trust and depend on. ABC Law Centers: Birth Injury Lawyers was just that.
- Michael


