Periventricular Leukomalacia (PVL) & Newborn Brain Damage
Premature babies are often admitted to the NICU because their lungs and other body systems aren’t fully developed. In addition, many premature babies experience a difficult course of delivery, making them susceptible to brain injuries. Preterm babies are especially susceptible to hypoxic-ischemic brain insults, which are insults caused by oxygen deprivation in the brain. Oxygen deprivation can be caused by a lack of oxygen in the baby’s blood and/or a restriction of blood flow in the brain. When premature babies suffer from oxygen deprivation and hypoxic-ischemic brain insults, they can develop a brain injury called periventricular leukomalacia (PVL). Although premature babies have a predilection for PVL, full term babies can also develop PVL as a result of oxygen deprivation. Periventricular leukomalacia can cause lifelong problems such as cerebral palsy, hydrocephalus, seizure disorders, developmental delays, intellectual disabilities and visual disturbances.
All babies, whether full-term or premature, that have signs of brain injury (usually called neonatal encephalopathy) are usually admitted to the NICU. In the NICU, babies are closely observed for signs of brain injury and associated problems, such as apnea (periods in which the baby stops breathing), respiratory distress, hypoglycemia and jaundice. Furthermore, seizures are very common in babies who have brain injuries, and the seizures usually start within the first 24 – 48 hours of life.
Babies suspected of having a brain injury will also have head imaging studies (pictures of the brain) performed so a brain injury can be diagnosed and the progression of the injury can be tracked. In addition, all babies who have a gestational age less than 33 weeks, or who have a birth weight less than 1500 grams, should have routine head imaging studies due to their susceptibility to brain injury. Periventricular leukomalacia often can be seen on an initial scan taken at 24 hours or later after the brain insult. Most cystic PVL can be detected by ultrasonography by 1 to 3 weeks. When abnormalities are detected, more frequent brain imaging should take place, and MRI (magnetic resonance imaging) is better at showing the extent of white matter injury.
In this article, we will discuss what periventricular leukomalacia is, what causes it, the signs and symptoms of PVL, how PVL is diagnosed and treated, and what to expect in the NICU and long-term for a baby who has PVL.
What Is Periventricular Leukomalacia (PVL)?
Periventricular leukomalacia is damage to the white matter of the brain, characterized by death (necrosis) of the white matter near the lateral ventricles, which are located in the top section of the brain. When the white matter tissue softens and dies, cysts filled with fluid may be left behind. The injured parts of the brain (lesions) in the periventricular region sometimes include hemorrhages (brain bleeds).
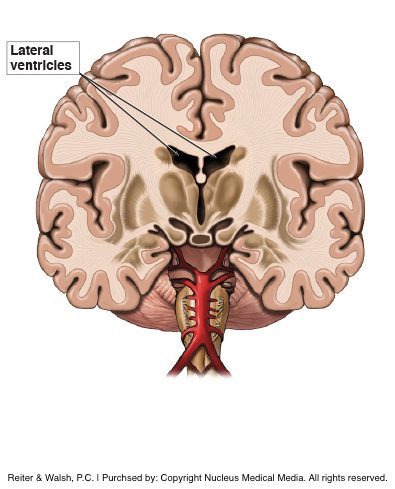
PVL can cause a child to have severe disabilities because the white matter plays a critical role in the functioning of the brain; it helps transmit messages throughout the largest part of the brain. When white matter dies, children may have motor, intellectual and visual problems. Spastic cerebral palsy with varying degrees of intellectual impairment – especially visual-motor dysfunction – is common in children who have periventricular leukomalacia.
What Are the Risk Factors for Periventricular Leukomalacia (PVL)?
In addition to prematurity, the risk factors for PVL are:
- Hypoxic events during or soon after birth
- Improper settings on the baby’s breathing machine (hypocarbia (low carbon dioxide in the blood))
- Moderate and severe brain bleeds (intraventricular hemorrhages (IVH))
- Lengthy resuscitation of the baby right after birth
- Maternal infections, such as GBS, and chorioamnionitis
- Infections in the baby, such as herpes encephalitis (HSV)
- Respiratory distress
- Pneumonia
- Low blood pressure
What Are the Causes of Periventricular Leukomalacia (PVL)?
Periventricular leukomalacia is caused by insufficient oxygen in the baby (hypoxemia and hypoxia) and/or restricted or decreased blood flow in the brain (ischemia). Events involved in the development of PVL are: 1.) decreased oxygen/blood flow to the periventricular region of the brain, and 2.) damage to glial cells, which are cells that support neurons; neurons are cells located throughout the brain and nervous system that process and transmit information through electrical signals. These two events can cause a cascade of events that leads to the development of PVL. White matter is mostly made up of glial cells.
Hypoxia and ischemia can cause PVL in both term and preterm babies, but the younger and smaller a baby is, the more prone she is to developing PVL. Babies at the highest risk of developing PVL are those under the age of 32 weeks gestational age. However, PVL can also form at term after brain insult.
There are a number of events that can cause hypoxia / ischemia and resultant PVL. Newborn blood vessels have very thin walls, and the vessels providing nutrients to the periventricular region cannot maintain sufficient blood flow during periods of low oxygen. In addition, low blood pressure caused by birth trauma, fetal distress, and post-birth hypocarbia and low blood pressure can lead to insufficient blood flow and oxygen in the baby’s brain. These hypoxic-ischemic events can cause damage to the blood brain barrier, a network of cells that regulates the flow of nutrients to the brain. An injured blood brain barrier can further contribute to greater levels of hypoxia. Injury to the blood brain barrier can also be caused by maternal infections that travel to the baby at birth. Premature babies are especially susceptible to these insults because their hearts, blood vessels and immune systems are not fully developed and they do not have the ability to auto-regulate blood flow in the brain.
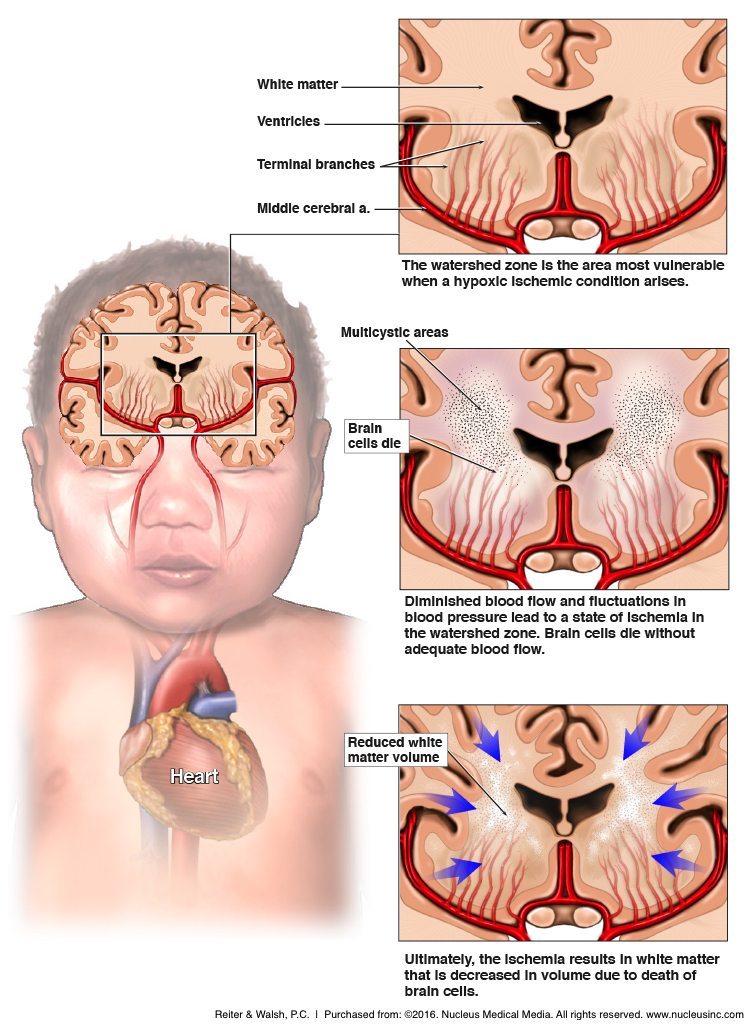
When hypoxic-ischemic injury or infection causes damage to the blood brain barrier, there is a cascade of inflammatory responses. One of these responses includes release of molecules called cytokines, which are toxic to the developing brain. Cytokines cause further brain injury by damaging nearby areas that were not involved in the initial injury. Additional damage is caused by free radicals, which are damaging molecules produced during ischemic episodes. Furthermore, when the glial cells become damaged, nearby neurons have little or no support.
Events during or near the time of birth that can lead to the development of PVL include the following:
- Ruptured uterus (womb)
- Placental abruption
- Preeclampsia / eclampsia
- Placenta previa
- Umbilical cord problems, such as a nuchal cord (cord wrapped around the baby’s neck), umbilical cord prolapse, short cord or cord in a true knot
- Failure to quickly deliver a baby when fetal distress is evident on the fetal heart rate monitor (delayed emergency C-section)
- Oligohydramnios (low amniotic fluid)
- Premature rupture of the membranes (PROM) / premature birth)
- Prolonged and arrested labor
- Intracranial hemorrhages (brain bleeds), which can be caused by a traumatic delivery. Forceps and vacuum extractors can cause brain bleeds. Sometimes intense contractions (hyperstimulation) caused by labor induction drugs (Pitocin and ) can cause head trauma. Mismanagement of cephalopelvic disproportion (CPD), abnormal presentations (face or breech presentation), and shoulder dystocia also put a child at risk of having a brain bleed.
- Hyperstimulation caused by Pitocin and Cytotec can also cause hypoxia that gets progressively worse.
- Fetal stroke
- Chorioamnionitis and infections in the mother that travel to the baby at birth. These maternal infections include the following: Group B Strep (GBS), herpes simplex virus (HSV), urinary tract infection (UTI) and bacterial vaginosis (BV).
- Improper management of the baby’s respiratory status after birth. This includes failure to properly manage apnea (periods of breathing cessation) and failure to properly manage a baby on a breathing machine (which can cause overventilation injuries, such as hypocarbia).
Signs and Symptoms of Periventricular Leukomalacia (PVL)
PVL is often silent, which means there are no signs, symptoms or encephalopathy. In some cases, PVL will not fully manifest until about 8 weeks after birth. Outward signs and symptoms are often not noticeable until much later, though, when the child starts to have more motor function and performs specific tasks. As the child misses certain developmental milestones, the extent of problems caused by PVL can start to be identified. As a newborn, feeding problems or unusual stiffness should cause concern regarding PVL.
Other signs and symptoms of PVL include the following:
- Weakness or abnormal muscle tone
- Vision problems
- Periods of apnea
- Low heart rate
- Seizures
- Delayed motor development (for example, babies may have all leg joints either flexing or extending)
Diagnosing Periventricular Leukomalacia (PVL)
PVL usually begins with numerous small areas of necrosis, followed by cystic formation and more spread out white matter injury (in more severe cases). Newborns typically have few or no signs of white matter injury, and PVL can easily be missed if routine screening is not performed. Prematurity, extreme stiffness, and/or poor ability to suckle should alert the physician that there may be white matter damage.
The initial diagnosis of PVL often is made using head imaging studies. Soon after an at-risk baby is born, physicians typically order an ultrasound to determine if the baby has white matter damage. However, the low sensitivity of an ultrasound allows for some white matter injury to be missed. MRI is much better than an ultrasound for identification of PVL. MRI can show noncystic PVL and very small lesions, while an ultrasound typically cannot. An MRI should be performed on babies who had a difficult course of development, especially if there was prematurity, maternal or fetal infection, a known hypoxic / ischemic event during or near the time of birth, or a traumatic head injury.
CT (computed tomography) scanning, is less useful for the diagnosis of PVL in very preterm babies because it detects fewer lesions than does MRI or ultrasound. In older babies, however, CT can identify the loss of periventricular white matter, and it can detect ventricular enlargement. Even with the best head imaging, however, some white matter damage can be missed and films can be interpreted as normal.
Listed below are important steps in identification of PVL:
- PVL often cannot be seen on an initial ultrasound scan in the first 24 hours after a brain insult; however, the scan will usually show periventricular damage when the baby is 24 hours old. If there are cystic changes, these changes will usually be seen after approximately 1 – 3 weeks. This emphasizes the importance of serial brain scans.
- Routine ultrasound screening should be performed on all infants with a gestational age less than 33 weeks – or with birth weight less than 1500 grams – to identify abnormalities in the brain. Screening should also be performed on all babies suspected of having a birth injury (such as a hypoxic-ischemic event) or birth trauma.
- Extremely low birth weight infants should have screening to detect IVH / brain bleeds.
- When brain abnormalities are detected, more frequent brain imaging studies should be performed to assess the progression of PVL.
- MRI should be used for better assessment of the extent of white matter damage. An MRI has better sensitivity and specificity than ultrasound and CT scans and can show brain injury at 1 day of age.
How Is Periventricular Leukomalacia (PVL) Treated?
Preventing premature birth is one of the most important steps in decreasing the risk of PVL. In addition, strategies that emphasize the maintenance of adequate blood supply and flow in the brain should be used to help prevent PVL. Low blood pressure, constricted blood vessels in the brain, and conditions that impair normal functioning of the blood vessels should be avoided. It is therefore essential to prevent hypocarbia, hypoxemia and abnormal blood pressure in a newborn baby.
No specific cure exists for PVL, but hypothermia (brain cooling) has proven very effective in treating infants with hypoxic ischemic encephalopathy (HIE). Hypothermia treatment has been shown to halt almost every injurious process caused by a hypoxic-ischemic insult. When administered within six hours of life, the treatment can prevent or reduce the severity of cerebral palsy, which is commonly caused by HIE.
Some research indicates that when a mother is given the steroid betamethasone during pregnancy, it can reduce the risk of PVL in the baby. In general, therapy for PVL focuses on teaching caregivers to handle, feed, dress, and toilet their children. Babies with PVL should be monitored for the development of disorders such as cerebral palsy, intellectual impairment, visual problems and epilepsy.
Short-Term and Long-Term Outlooks for Babies with Periventricular Leukomalacia (PVL)
While in the NICU, babies with PVL may have apnea, difficulty feeding, an inability to control facial movements, decreased tone (limpness) in their lower extremities, neck stiffness and seizures. Newborns with PVL are also usually irritable. Once children with PVL are older, they are likely to miss certain developmental milestones due to motor problems and intellectual disabilities. Visual-motor dysfunction is common and many children with PVL are diagnosed with spastic cerebral palsy.


ABC Law Centers: Birth Injury Lawyers | Legal Advocates for Children with Disabilities
If you are seeking the help of a lawyer, it is very important to choose a lawyer and firm that focus solely on birth injury cases. ABC Law Centers: Birth Injury Lawyers is a national birth injury law firm that has been helping children for almost 3 decades.
If your child was diagnosed with a permanent disability such as PVL, cerebral palsy, a seizure disorder, intellectual disabilities or developmental delays, the award winning periventricular leukomalacia (PVL) lawyers at ABC Law Centers: Birth Injury Lawyers can help. We have helped children throughout the country obtain compensation for lifelong treatment, therapy and a secure future, and we give personal attention to each child and family we represent. Our nationally recognized firm has numerous multi-million dollar verdicts and settlements that attest to our success and no fees are ever paid to our firm until we win your case. Contact ABC Law Centers: Birth Injury Lawyers for a free case evaluation. Our firm’s award-winning lawyers are available 24 / 7 to speak with you.
Featured Videos
Posterior Position
Hypoxic-Ischemic Encephalopathy (HIE)

Featured Testimonial
What Our
Clients Say…
After the traumatic birth of my son, I was left confused, afraid, and seeking answers. We needed someone we could trust and depend on. ABC Law Centers: Birth Injury Lawyers was just that.
- Michael
Helpful resources
- Deguchi K & Miller G.Periventricular leukomalacia. In: UpToDate. Dashe JF (Ed), UpToDate, Waltham, MA, 2014.
- Owens R. Intraventricular hemorrhage in the premature neonate. Neonatal Netw 2005; 24:55.
- Kenet G, Kuperman AA, Strauss T, Brenner B. Neonatal IVH–mechanisms and management. Thromb Res 2011; 127 Suppl 3:S120.
- Volpe, JJ. Neurology of the Newborn, 4th ed, WB Saunders, Philadelphia 2001.
- Kinney HC. “The near-term (late preterm) human brain and risk for periventricular leukomalacia: a review.” Semin Perinatol 2006; 30:81.
- Woodward LJ, Anderson PJ, Austin NC, et al.” Neonatal MRI to predict neurodevelopmental outcomes in preterm infants.” N Engl J Med 2006; 355:685.
- Khwaja O, Volpe JJ.” Pathogenesis of cerebral white matter injury of prematurity.” Arch Dis Child Fetal Neonatal Ed 2008; 93:F153.
- Volpe JJ. “Encephalopathy of prematurity includes neuronal abnormalities”. Pediatrics 2005; 116:221.


