What are long-term effects of brain bleeds?
Certain types of brain bleeds are small and may not have long-term effects. However, a severe or poorly managed brain bleed can cause permanent damage to the brain. Long-term effects may affect important areas controlling cognition, motor skills, and memory.
Long-Term Effects of Brain Bleeds
Some brain bleeds in babies have been proven to cause long-term cognitive and behavioral effects. During a brain bleed, areas of the brain can be deprived of oxygen-rich blood. Even a short time without oxygen can cause serious injury to the brain. Swelling after a brain bleed can damage blood vessels and crucial brain tissue.
Without enough white matter in their developing brains, children may lack control of their basic bodily functions. Brain bleeds can also harm the cerebral cortex, which is crucial to memory, attention, thought, language, and consciousness.
After a brain bleed and resulting brain injury, a baby’s brain may have irreversible damage. The child may develop:
- Cerebral palsy and other motor disorders
- Seizures and seizure disorders
- Hearing impairments
- Vision impairments
- Developmental delays
- Learning disabilities
- Cognitive impairment
- Speech delays
Side Effects of Brain Bleeds
Water on the Brain (Posthemorrhagic hydrocephalus)
A common complication of more severe infant brain bleeds is posthemorrhagic hydrocephalus, or fluid buildup in the brain. Hydrocephalus has many potential long-term effects.
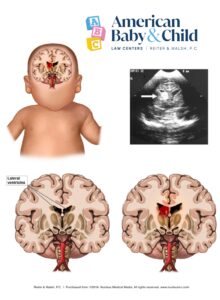
Posthemorrhagic hydrocephalus , sometimes inaccurately called “water on the brain,” is a condition in which too much fluid builds up around the brain.
After a brain bleed, cerebrospinal fluid collects in brain ventricles and subarachnoid spaces around the brain. The resulting swelling can damage blood vessels and the brain’s white matter. White matter regulates activity throughout the nervous system.
Hydrocephalus can cause many potential long-term effects.
Detecting Hydrocephalus
Hydrocephalus can be detected early through brain imaging. Later, obvious clinical signs occur, such as increasing head circumference. Early detection allows medical professionals to prevent further injury to the brain.
As the ventricles continue to enlarge, they put pressure on nearby brain tissue, potentially causing permanent brain damage. The long-term effects of neonatal brain damage depend on how severe the damage is and how it is handled. Poor treatment and recovery can lead to serious and life-long disabilities.
Tell us your story.
Dealing with a birth injury diagnosis can be difficult, but our attorneys can help. The ABC Law Centers: Birth Injury Lawyers team focuses exclusively on birth injury and are dedicated to earning justice for families like yours.
Brain bleeds and birth trauma
A leading cause of infant brain bleeds is hypoxic-ischemic encephalopathy (HIE). HIE isa type of injury resulting from a traumatic birth when a baby does not get enough oxgyen. HIE decreases the amount of oxygenated blood in certain areas, sometimes causing brain damage and hemorrhage.
Brain bleeds can also result from the use of tools like forceps or vacuum extractors, in cases where the baby gets stuck in the birth canal. This can also cause trauma to the head and brain and result in hemorrhage.
Infant brain bleeds from medical malpractice
A number of medical mistakes and deviations from standards of care can cause brain bleeds in babies. If medical staff neglects to act quickly and an injury occurs, it may be medical malpractice.
It can be difficult to learn that malpractice or negligence caused harm to your baby. Parents put their trust in healthcare staff. A brain bleed diagnosis and a long stay in the neonatal intensive care unit (NICU) is taxing on families.
Our Birth Injury Attorneys Can Help
If you suspect that your loved one suffered a brain bleed as the result of medical malpractice, reach out to the team at ABC Law Centers: Birth Injury Lawyers. We focus exclusively on families like yours. Our attorneys exclusively handle birth trauma cases and have specifically handled cases involving brain hemorrhages from medical malpractice.
Call us today for a free case review. We are ready to hear your story and answer any questions you may have about your child’s future.
The information presented above is a general educational resource. It is not medical advice. If you have questions a diagnosis of infant brain hemorrhages or posthemorrhagic hydrocephalus, please consult with a medical professional.
Related Resources
Sources
- Periventricular/Intraventricular Hemorrhage (PVH/IVH) in the Premature Infant
- Management and complications of intraventricular hemorrhage in the newborn
- Intraventricular hemorrhage in term neonates with hypoxic-ischemic encephalopathy: a comparison study between neonates treated with and without hypothermia